Gingival Recession
Gum or Gingival Recession (receding gums) is the result of trauma to the gum as a result of toothbrush abrasion or other trauma or changes induced by bacterial associated inflammation, such as gum disease. The major genetic susceptibility is associated with the width of the gum tissues or what is described by dentist as the gingival biotype. Gum recession is a common problem in adults over the age of 40, but it frequently occurs in the teens and following orthodontics.
Causes
The major causes of gingival recession are:
- Gum or Periodontal disease. Accumulation of dental plaque due to inadequate brushing and interproximal cleaning, may lead to painless, chronic inflammation of the gums and gradual recession.
- Overaggressive brushing will also induce inflammation in the gum in much the same way as the bacterial plaque does.
- Hereditary thin, fragile or insufficient gingival tissue predisposes to gingival recession (The thin biotype).
- Self-inflicted trauma, such as habits like digging a fingernail or pencil into the gum.
- Orthodontic movement of teeth which results in the development of a thin gum situation over a misaligned tooth.
- Abnormal tooth position due to crowding may have the same effect as orthodontic misalignment.
- Piercings in the lip or tongue that abrade the gum.
Symptoms
Gum recession is generally a slowly developing event and subsequently is more pronounced in older individuals. Receding gums may remain unnoticed until the condition starts to cause symptoms and these are:
- Dental Hypersensitivity.
- Teeth that appear longer than normal and the roots of the tooth are visible.
- The tooth feels notched at the gum line
- Change in the tooth’s colour (due to the colour difference between enamel and dentine)
Mechanism
The epithelium or covering layer of the skin is made up of epithelial cells and the underlying connective tissue. For example the skin on the back of the hands is different from the palms of the hand yet the epithelial cells are the same. What makes the difference is the underlying connective tissue. When the connective tissue is inflamed, the inflammation will induce a thickening of the epithelial cell layer in an attempt to protect the tissue. The way the body does this is by resorbing the connective tissue underneath the epithelial cells to produce indentations (rete pegs). This in reality simply increases the number of dividing cells and hence an increase in the skin thickness. The rete pegs can be seen in the Gum, Thin skin and Thickened skin in the micrographs to the right. If the tissue is thin then the loss of the supporting connective tissue will result in recession of the gum as we lose the connective tissue support.
Treatment
Cause related: Treatment should start with addressing the cause of the problem. If excessive brushing is the cause, the patient should consider using a softer brush, changing the action of brushing and/or changing to an electric brush so that they can eliminate the old habit of brushing. Alternatively if poor oral hygiene is the cause improved cleaning along with removal of the hardened plaque (Calculus/tartar) should occur.
Symptom related: Once the cause associated treatment is addressed than consideration can be given to treating the recession if there are aesthetic issues with the site (Does the gum look different – is it unacceptable for the patient?). Is the treatment method to be used successful and does it have good long term outcomes to justify the expense? Gingival grafting is the usual method used.
We will discuss all these issues with you and together we will come up with an appropriate treatment plan for you.
© Penam Investments Pty Ltd 2020.
Translate This Page
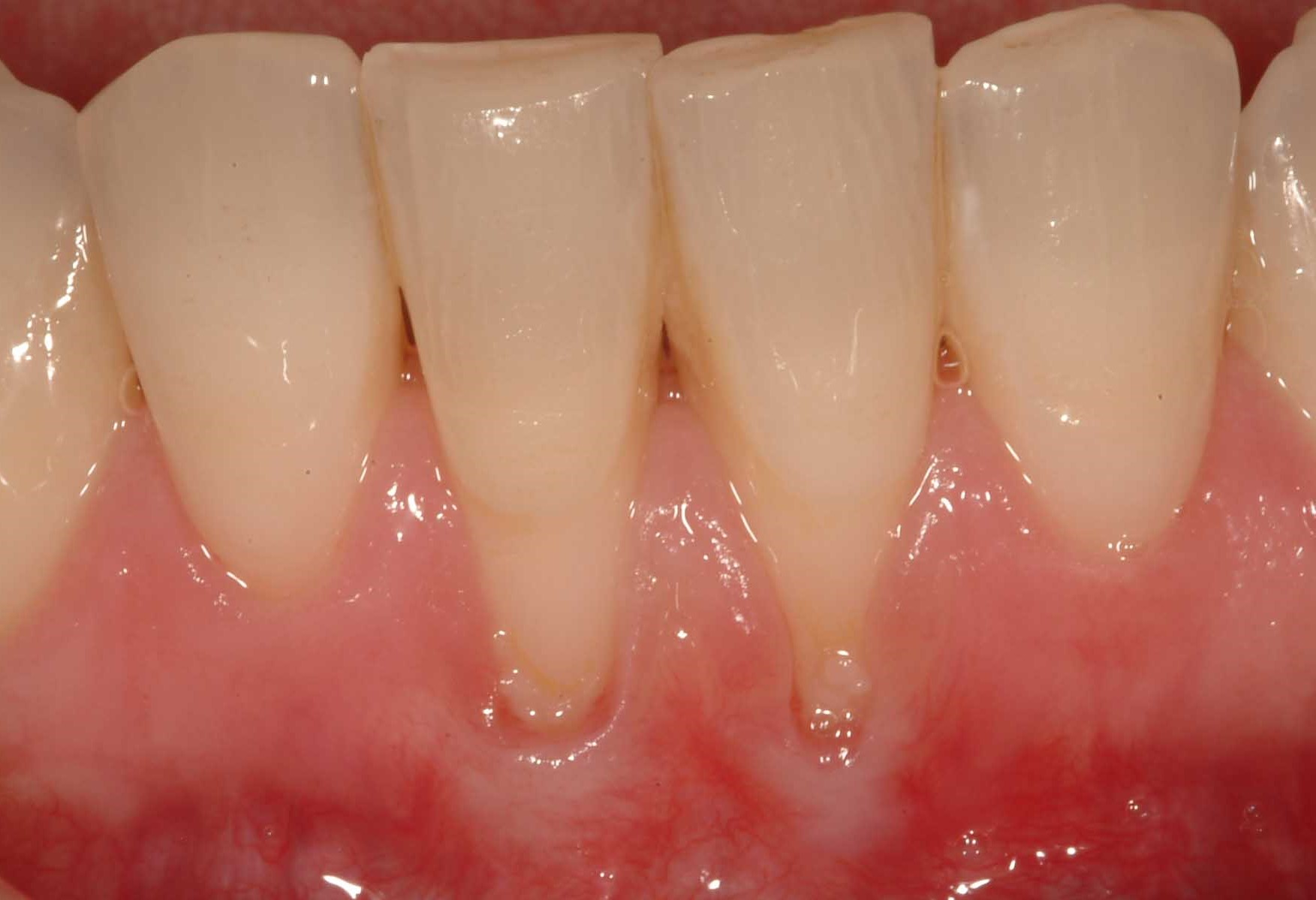
Photo of receded gum around the lower incisors. These teeth have thin gum tissue and dental plaque inducing inflammation at the base of the receded area. The gum at the base of the areas has a whiter appearance – most likely from the skin becoming thicker.
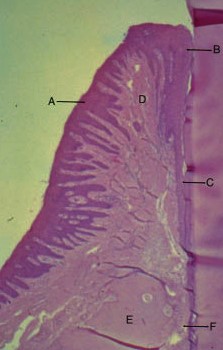
The Gingiva (gum). The dark purple area is the epithelial or covering cells. The purple indentations on the tissue side of the epithelial cells are called “Rete pegs”. This micrograph shows that the Rete pegs are deep and occur on both sides of the gum. Against the tooth and on the outer surface.
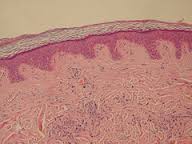
Micrograph of normal skin on the arm or trunk. This thin skin has short Rete pegs and if subject to inflammation induced by trauma or friction will stimulate the epithelium to become thicker. To do this the skin resorbs the connective tissue underneath which makes the Rete pegs longer as seen in the micrograph below.
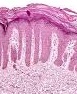
Long Rete pegs with thickened skin. The flaky material on the skin surface is the thickened epithelial layer. If the gum is thin than the loss of the connective tissue will result in recession.